Proposed Change to Brain Death Laws Draws Criticism from Some Doctors, Ethicists
Catholic doctors and ethicists today largely echo St. John Paul II in stating that brain death, when properly diagnosed, is not a “kind” of death; it is simply death, period.

WASHINGTON — A proposed change to U.S. law concerning the determination of brain death has drawn criticism from a group of doctors, lawyers, and philosophers, who say that the proposed changes, among other things, could lead to incorrect diagnoses of brain death in patients who are in fact still alive.
In a statement published May 14 in the Journal of Medicine and Philosophy, a group of over 100 “experts in medicine, bioethics, philosophy, and law” affirmed that while the law regarding brain death does need revision, a proposed revision known as the RUDDA “is not the way to do it.”
Several Catholic doctors and ethicists have the signed the statement.
“We span a wide range of professions, world views, and nationalities,” the statement reads.
“We do not necessarily agree with each other on all aspects of the brain-death debate or on fundamental ethical principles. We do agree that the UDDA needs to be revised and that the RUDDA is not the way to revise it.”
The RUDDA is one proposal currently under consideration by a study committee of the nonprofit Uniform Law Commission, convened during August 2020.
If the Uniform Law Commission decides to accept the RUDDA, state legislatures across the country could follow suit in adopting the revised law.
What is brain death?
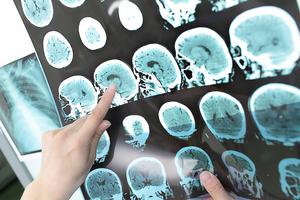
Brain death, also called death by neurological criteria, is the practice of declaring a person dead based on the loss of brain function, rather than the stoppage of the heart and breathing.
Brain death is a commonly accepted standard for declaring a person dead, and is used by doctors dozens of times every day throughout the United States. According to the 1981 guidelines of the American Medical Association, brain death entails the “irreversible cessation of all functions of the entire brain.”
Brain-dead donors are, today, the primary source of organ transplants. Organs such as the heart, lungs, and pancreas can be— and are— harvested from brain dead donors as close to the time of death as possible.
While the term “brain death” is not found in the Catechism of the Catholic Church, St. John Paul II asserted in 2000 that, if properly diagnosed, the complete and irreversible cessation of all brain function seems a valid way to assess with moral certainty that a person has died.
Catholic doctors and ethicists today largely echo St. John Paul II in stating that brain death, when properly diagnosed, is not a “kind” of death; it is simply death, period. However, brain death remains a hotly debated topic among some Catholic medical professionals and ethicists.
What is the proposed legal change?
Authors Ariane Lewis, Richard Bonnie and Thaddeus Pope proposed several revisions to the Uniform Determination of Death Act — a 1981 law that all U.S. states have since adopted— in a January 2020 article published in the Annals of Internal Medicine.
Lewis, Bonnie, and Pope say one of the reasons for their proposed RUDDA is that there is confusion about what constitutes “accepted medical standards” for declaring a patient brain dead.
Thus, the RUDDA would bring the law in line with guidelines for diagnosing brain death put forth by the American Association of Neurology.
However, the AAN guidelines— last updated in 2010— do not mandate tests for complete cessation of brain function beyond what can be diagnosed bedside, such as an electroencephalogram.
The authors further suggested a revision to a sentence in the UDDA which currently mandates “irreversible cessation of all functions of the entire brain” as a criterion for brain death, most notably deleting the word “all.”
This is because hormonal function, associated with the part of the brain called the hypothalamus as well as the pituitary gland, is not part of the “accepted medical standards” for brain death, the authors claim.
The authors thus suggest adding “with the exception of hormonal function” to the UDDA’s “entire brain” requirement.
Finally, the proposed revisions would remove any need for doctors to obtain consent from a patient’s family members before performing brain death tests.
Why has the RUDDA faced opposition?
The signers of the May statement point out three reasons why, in their view, the RUDDA proposed by Lewis, Bonnie, and Pope ought not be adopted into law.
Pointing to rare cases where patients diagnosed as brain dead have continued to live— sometimes for years— the signers asserted that the RUDDA could lead to “a non-negligible risk of misdiagnosing a live patient as dead.”
The National Catholic Bioethics Center has said in the past that in cases where a patient declared brain dead has ultimately recovered or improved indicates an incorrect diagnosis of brain death in the first place.
“Stories of people continuing on a ventilator for months or years after being declared brain dead typically indicate a failure to apply the tests and criteria for determination of brain death with proper attentiveness and rigor,” said Fr. Tad Pacholczyk, director of education for the center, in a 2005 information sheet.
“In other words, somebody is likely to have cut some corners in carrying out the testing and diagnosis.”
The signers also rejected Lewis, Bonnie, and Pope’s claims that a patient can be declared brain dead despite continuing hypothalamic, or hormonal, function.
Excluding hormonal function from the definition of brain death would remove the ability to sue from families or proxies of patients who continue to grow despite being declared brain dead.
One highly publicized case is that of Jahi McMath, a 13-year old California girl who in December 2013 suffered a brain hemorrhage after complications following routine tonsil surgery.
Five physicians- two at Children’s Hospital Oakland and three independent doctors requested by the family- declared McMath brain dead based on tests showing no blood flow to her brain and no signs of electrical activity after performing an EEG.
McMath’s family contested the diagnosis, and in January 2014 the hospital released her. The girl’s family took her to an undisclosed location— reportedly in New Jersey— for treatment where, the family claims, McMath continued to live and grow, even undergoing menstruation.
“[I]t is simply absurd to propose that periodic menstruation is compatible with being dead,” the statement authors assert.
Videos posted online show McMath occasionally exhibiting movement, such as twitching her foot. In June 2018, McMath’s family said that the teenager had died, citing “complications associated with liver failure.”
Finally, the signers of the May statement criticized the RUDDA’s proposal that informed consent is not needed for certain confirmatory brain death tests, such as an apnea test, whereby a patient is removed from a ventilator for several minutes to see if they are capable of breathing on their own.
The signers cited evidence that apnea tests are non-beneficial to patients and can, at least in theory, actually precipitate brain death rather than test for it.
The signers conclude the statement by arguing that a revised law ought to include an opt-out clause for people who do not accept brain death on religious or other grounds.
“Objections to a neurologic criterion of death are not based only on religious belief or ignorance. People have a right to not have a concept of death that experts vigorously debate imposed upon them against their judgment and conscience,” the authors assert.
“This is not to say that anyone should be able to specify any fanciful concept of death for themself, but yes, that anyone should be able to specify that they want to be declared dead by circulatory-respiratory criteria rather than by neurological criteria.”
What should Catholics make of this?
While organ donation and acceptance is allowed and even laudable for Catholics, care must be taken to ensure that the donor is in fact dead.
The NCBC states that it is acceptable for Catholics to receive transplanted organs from brain dead donors, as long as there is moral certainty that the diagnosis has been made with “rigor.”
In his 2000 address, St. John Paul II stressed the importance of only removing organs from people who have definitively died.
The pope’s speech built upon his writing in the 1995 encyclical Evangelium vitae, in which he decried any practice whereby “organs are removed without respecting objective and adequate criteria which verify the death of the donor,” calling such a practice a form of “furtive...euthanasia.”
Dr. Joseph Eble, a private practice doctor and president of the Tulsa Guild of the Catholic Medical Association, told CNA in April that he worries that a shift away from anything less than the most rigorous standards for diagnosing brain death could make it harder for Catholics to be morally certain that a person has in fact died.
Eble added that he worries that making confirmatory tests optional under law will make it easier for doctors to diagnose brain death in patients who have a chance of recovery if their organs were not harvested and they were given additional time.
Jozef Zalot, a staff ethicist for the National Catholic Bioethics Center, told CNA in April that while in principle having uniform guidelines is a good thing, it is worth asking whether the AAN guidelines, as proposed by the authors of the revisions, are the best guidelines to use.
The proposed changes to the UDDA seem, Zalot said, to militate against moral certitude that a person is dead by making certain confirmatory tests unnecessary.
“It certainly gives the appearance of cutting corners,” he said.
Dr. Barbara Golder, a medical doctor and lawyer with the Catholic Medical Association, noted that brain death often does not “look” like death, as a patient declared brain dead may still appear to be breathing, exhibit involuntary functions such as sweating, and may even grow and develop.
The bodies of brain-dead patients are sometimes given anesthetics while their organs are harvested, and may exhibit involuntary movements.
The Pontifical Academy of Sciences addressed this phenomenon in a 2008 paper, stating that “the ventilator and not the individual, artificially maintains the appearance of vitality of the body. Thus, in a condition of brain death, the so-called life of the parts of the body is ‘artificial life’ and not natural life. In essence, an artificial instrument has become the principal cause of such a non-natural ‘life’. In this way, death is camouflaged or masked by the use of the artificial instrument.”
The National Catholic Bioethics Center agrees, stating that despite the complete loss of brain function, “artificial support may cause the victim to appear alive visually and to the touch.”
The Pontifical Academy of Sciences also stated that “brain death...‘is’ death,” and that “something essential distinguishes brain death from all other types of severe brain dysfunction that encompass alterations of consciousness (for example, coma, vegetative state, and minimally conscious state).”
“If the criteria for brain death are not met, the barrier between life and death is not crossed, no matter how severe and irreversible a brain injury may be,” the academy added.
Golder stressed that Catholics are not obliged to continue futile care. She told CNA that in general, for most situations, a brain death diagnosis is both “reliable and reasonable” when it is used to determine whether to cease care, such as a ventilator, to a patient.
Still, making the decision to discontinue treatment to a loved one and let an illness run its natural course— whether the patient has been declared brain dead or not— is never easy, and should be done in close collaboration with a trusted doctor, she said.
“Don’t be shy about asking for someone to help guide and interpret. It’s really important,” she said.
“Ask the doctor to explain how the process [of declaring brain death] works, as different places have different protocols. There are no ‘silly’ questions—ask whatever comes to mind.”
Catholic families should understand that most doctors are doing the best they can when it comes to diagnosing death. The rest, she says, is in God’s hands.
- Keywords:
- brain death
- medical ethics
- RUDDA