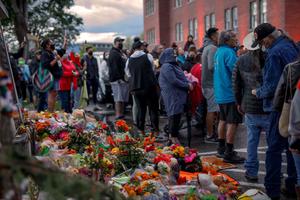Catholics Engaged in the Global Fight against COVID-19
Catholics from around the world told the Register their stories of being on the hospital frontlines of COVID-19.

MUMBAI, India — Fear gripped India’s largest city under lockdown. With nearly the same area of New York City, and with one and half times the population, Mumbai was seeing COVID-19 ravage the city and turn its hospitals into battlefields. And like a general on the frontlines, Sister Beena Madhavath, herself a medical doctor, was staring down the face of panic in her own medical department at Holy Family Hospital.
During one particularly chaotic day of treating the flood of patients, the entire department at Holy Family Hospital — nurses, doctors, and maintenance staff — threatened to resign. Fear was more contagious than the coronavirus.
“Fear is a common factor, but this is a time for courage,” Sister Beena, of the Order of Ursulines of Mary Immaculate and the hospital’s assistant executive director, told her department. In the course of a 45-minute discussion she assured them they would have the PPE (personal protective equipment) they needed to be safe in caring for patients, and they would be taken care of should anything happen to them.
She pointed out to her staff that staying at home in their densely populated city, where they would have to mingle with the population anyway to get the basic necessities of life, would not make them any safer from the virus than working at the hospital with all their protective measures in place.
“We have equal risk whether you’re inside or outside,” she said, recounting this experience to the Register.
India: Christian Courage to Fight
Since March, Holy Family Hospital has been working to try to keep Catholic health care serving people. In India, there are three main options: corporate hospitals for the wealthy who can afford them; government hospitals for the poor who can’t afford the corporate hospitals: and Christian hospital alternatives who try to provide quality care to all.
“We offer compassionate and quality care so the common man can come to our center for treatment,” Sister Beena said.
Pointing to one of countless examples, Sister Beena explained the hospital had to provide care for one pregnant woman who had to deliver her baby and was suspected to have COVID. Staff created a makeshift isolation room, and then arranged a transfer after the birth because their facilities could not care for both a mother and child.
Some cases Holy Family’s staff receives are more complex. They had one patient who needed both a ventilator and dialysis, and difficulty finding a hospital with both machines and an isolated ICU to care for him.
“We had to shift from one [health care facility] to another,” Sister Beena said.
Still, she is happy that so far 50% of their COVID patients have recovered.
But part of the battle is keeping people calm through the prolonged crisis. Holy Family has provided its staff access to a counselor to help them through the stress. The patients are agitated as well. The staff had a couple incidents where they needed to get the help of the police.
But Sister Beena sees hope.
“I feel God’s protection and direction in my life,” she said.
Holy Family Hospital is part of the Catholic Health Association of India (CHAI), a network of 500 Catholic hospitals that have been key collaborators with India’s government from the outset of the crisis. India has 1,000 nuns alone who, like Sister Beena, are trained medical doctors. CHAI conveyed that it was critical for the government to make sure all health care workers had full protective gear, which was difficult to obtain at the outset.
“Otherwise the fight against COVID-19 could not be sustained,” explained Father Mathew Abraham, CHAI’s director general and himself a medical doctor.
CHAI has also helped secure and distribute material resources, conduct training in using PPE, assembled food kits, and developed stringent protocols needed for the fight against COVID-19 in India.
In India the national lockdown was necessary to prevent the hospital system from immediate collapse. It helped slow the infection down enough to prepare to handle COVID cases coming in. The southern Indian state of Kerala, Father Abraham explained, has done the best job in India at being proactive in dealing with COVID-19, but the same cannot be said of other states.
“The curve is not flattened” in India, he said. “It is going to go up.”
According to Father Abraham, because India does not have a robust social safety net compared to Western Europe or the United States and Canada. The national lockdown has been extended until May 31, and many people are being sunk financially by the virus, either by not having work or by trying to pay for health care. In consequence millions of migrant workers are now in the midst of an exodus from the cities, undaunted by travel restrictions. They have learned of people walking almost 300 miles to return to their home villages.
“Many of them took the infection back with them,” he said.
Father Abraham said he is worried — and for good reason. The Indian government has eased travel restrictions in advance of the lockdown’s anticipated May 31 ending, but COVID-19 cases are rising. India’s hospitals face a catastrophic situation, similar to what some U.S. hospitals have been experiencing, since like their U.S. counterparts India’s hospitals have also canceled elective surgeries to deal with the surge of highly contagious COVID patients. As a result of this shift in focus, at Holy Family Hospital in Mumbai, revenues are down 70% and expenses have doubled.
Without financial support, Father Abraham said, the question is “How many Catholic hospitals will survive and for how long?”
Liberia: Lessons from Ebola
The ravages of civil war followed by a draining battle against an Ebola outbreak had left Liberia’s health care system in a fragile state by the time COVID-19 arrived. Catholic health care clinics have been engaged since in an ongoing fight to save women dying from childbirth and infants from succumbing to diseases long wiped out in developed countries by vaccines, modern sanitation and clean water those populations now take for granted.
At the outset of the crisis, the health care system was not able to cope, Franciscan Missionary of Mary Sister Barbara Brillant, a health care worker in Monrovia, told the Register. Staff at the clinic she served immediately had to triage cases, and sending suspected patients with COVID to the 14th Military Hospital in Schiefflin Town, which was far better equipped to handle advanced COVID-19 cases, was not easy.
Sister Brillant said her clinic tried to send one extremely sick and semi-conscious patient to the military hospital for advanced care.
“The hospital said we can’t take this patient or else he’ll infect our whole hospital,” she said. She worked the phone trying to get someone up the chain of command at the military hospital to take the patient. Meanwhile the seconds ticked away for the patient, who was already loaded into an ambulance waiting for word to go.
“It took almost two hours of this patient lying in the ambulance for [the military hospital] to respond,” Sister Brillant said. Finally, the medical officer in charge of the military hospital came down and personally transferred the patient from the clinic’s ambulance to a military ambulance and transported him to the military hospital.
Sister Brillant thought Liberia’s recent battle against Ebola would have set the country up well to deal with COVID-19.
But, she said, “COVID is totally different because it’s not so obvious to people that it’s real.”
“With Ebola, people were bleeding, dying, the bodies were on the streets. … You could see it,” she added. “And this COVID you don’t see.”
On the one hand, they had a good amount of heavy PPE left from the Ebola fight. But on the other, they discovered that their ability to resupply was heavily strained. The developed world was in a mad scramble for PPE to fight back major COVID outbreaks. The countries that had once poured in massive amounts of funds to combat Ebola, now had little to offer Liberia.
“You cannot buy gloves, you cannot buy masks, and who’s going to export anything to us?” Sister Brillant said.
But a new problem her clinic has seen emerge is that people are getting afraid to go to the hospital, even though 14th Military Hospital, which is the only hospital in Liberia accepting COVID-19 patients, has proven itself to offer the best chances of survival. Many people instead are suffering and dying from the disease at home. And some respond violently out of fear or suspicion: One clinic in a rural village was attacked because people learned the clinic’s isolation unit had eight patients under observation for COVID-19.
Sister Brillant said Liberia is testing the dead to gauge how extensively COVID-19 has spread.
“We’re one of the few countries in Africa that are testing dead bodies,” she said. “That is a lesson we learned in Ebola.”
But people all over the world, she said, are being infected by fear, and the world will have to find a way to deal with the trauma. She said they are trying to communicate with the people, especially over radio. “There is something to be fearful about,” Sister Brillant said, “but nothing to be fearful about if we do the right things.”
Haiti: Helping People Protect Themselves
Anselm Joseph recounted the day they discovered COVID-19 had arrived in the south of Haiti around the city of Les Cayes. A Haitian man had fallen ill and carried the virus with him from the nation’s capital, Port-au-Prince, back to his village in the vicinity of Joseph’s health clinic, the Klinik Fronfrèd. He came into the Klinik Fronfrèd, situated just outside Les Cayes, with a host of flu-like symptoms, but one symptom immediately stood out as a telltale of COVID-19 infection: he had no sense of smell or taste.
Anselm Joseph a Haitian Catholic who is a special projects director with the Gaskov Clergé Foundation, a non-profit that oversees the operations of Klinik Fronfrèd, told the Register this man had to be hidden from the public straightaway.
“His identity had to be hidden from the community for his own protection,” he said. The community had to be protected from the curious who wanted to see what a person with COVID looks like.
Joseph said Haiti is extremely vulnerable in dealing with advanced cases of COVID-19. Haiti’s largest hospital in Port-au-Prince, he explained, is already at maximum capacity. The south of Haiti, he said, has one hospital with a capacity for 40-50 COVID-19 patients.
At his clinic, he said, “We’ve been pushing to rehab an old hospital building from back when [tuberculosis] patients had to be hospitalized.” Once the initial renovations to the building are finished, the Klinik Fronfrèd will have to equip it.
But the Klinik Fronfrèd faces a daunting challenge with severe cases of COVID-19. Unlike medical facilities of countries in the developed world, Haiti has little advanced hospital care to save lives if COVID rapidly advances. The country itself in total has an estimated 124 ICU beds and 64 ventilators total for a population of 11 million. Joseph explained his clinic is not equipped with ventilators, and even if they had them, they do not have trained respiratory therapists to operate them safely.
“We’re not ready, that’s for sure,” he said.
Other clinics have closed because they did not have PPE to protect their staff. But Joseph said Klinik Fronfrèd has remained open, but at reduced capacity to maintain social distancing. The clinic added outdoor tents and isolation wards. The staff also went to their warehouse and looked at what they had, and determined they had gowns and hairnets and n95 masks to stay open — for now.
But Joseph said the situation is grave. He calculated that they have about 1-2 weeks left of PPE in storage.
“If we are closed, then we’d be killing people, not COVID,” he said, noting they have patients with diabetes, heart and lung conditions or nutritional issues, for example, that cannot afford to go without care. And without that continuing care from Klinik Fronfrèd, “If these people did get COVID, they would not make it.”
The country has only one agency running the tests for COVID-19, but not all clinics are taking the needed precautions to keep suspected COVID patients in isolation.
“At other clinics they just leave [after the test] and re-enter the general population,” he said.
The main challenge is convincing people that the threat is real, when “they don’t see people dying unless it is on TV.”
“We haven’t seen a change in the behavior of the population,” Joseph said.
The clinic employs four permanent doctors, four on-call doctors, and six nurses on staff. Joseph said they try to keep calm but it is a constant challenge as the medical staff realize that they have less protective gear available to them than medical staff in places like New York City who are also severely challenged by the virus.
“[Our medical personnel] watch TV, they see social media, and they see what equipment their counterparts are using in the developed world and they’re still getting infected,” he said.
Joseph said Haiti’s only hope is to raise awareness through the country about the risks.
“That’s more important than the medical part of this,” he said. “The best we can do is give people the means to protect themselves.”
As a sign of hope, their clinic’s first COVID-19 patient is now almost recovered, Joseph said. As one sign that this patient is on his way to better health, he could now finally smell a perfume applied to the back of his hand.
Peter Jesserer Smith is a Register staff writer.
MORE INFO
To aid the charities in this story, go to Catholic Relief Services’ has a COVID-19 Response website.
- Keywords:
- catholics
- coronavirus
- india