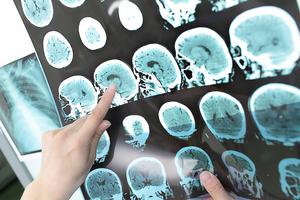
Doctors Push to Allow Death by Organ Donation
A recent study claims the majority of Americans would support ditching the ‘dead-donor rule’ for organ extraction.

ARLINGTON, Texas — Cases like that of Martha Perez, a 26-year-old woman whose family said they felt pressured to donate her organs in Arlington, Texas, last month, following a tragic car crash, highlight public uncertainty about the medical definition of “brain death.”
“But she still has heart and lung functions,” family member Juan Martinez told MyFoxDFW.com before her organs were harvested. “They took her off life support, and she was still breathing. My family feels pressured, and it’s just hard for someone to make that kind of decision when this just happened.”
To avoid public confusion over complicated definitions like “brain death,” some doctors and bioethicists are now saying it would be better — and more “honest” — to simply allow the killing of patients by surgically removing their vital organs. The so-called “dead-donor rule” — the long-held ethic that says doctors must not end their patients’ lives by extracting their organs — is not followed in practice anyway, say the critics, so why have it?
And, according to a recent poll published in the British Medical Journal, more than 75% of Americans support harvesting patients’ vital organs — even if it kills them.
“Brain-dead organ donors are the principal source of transplantable organs. However, it is controversial whether brain death is the same as biological death,” said the study, "Abandoning the Dead-Donor Rule? A National Survey of Public Views on Death and Organ Donation. “Therefore, it is unclear whether organ removal in brain death is consistent with the ‘dead-donor rule,’ which states that organ removal must not cause death.”
The study’s lead author, Florida State University College of Medicine philosopher/ethicist Michael Nair-Collins, and his colleagues conducted an Internet survey of 1,096 Americans. Those surveyed were presented with a “vignette” of a man in an irreversible coma following a car accident who is unaware, cannot feel pain and has previously consented to organ donation.
“Of the 85% of the sample who agreed that they were willing to donate organs after death, 76% agreed that they would donate in the scenario of irreversible coma with organ removal causing death. There appears to be public support for organ donation in a scenario explicitly described as violating the dead-donor rule,” the study concluded.
‘Brain Death’ Challenged
Nair-Collins justifies harvesting organs from living persons, in part, by attacking the legitimacy of the concept of “brain death” that is utilized in some cases to define a person as dead even though some basic life functions remain operative.
“Patients who have been accurately diagnosed with ‘brain death’ according to accepted standards are able to engage in a large variety of integrative, feedback-driven biological functions that work together to maintain the internal physiologic stability for the organism as a whole and can do so over very long periods of time,” Nair-Collins told the Register.
“This includes things like getting a fever in response to an infection, healing wounds, regulating the amount of salt and water in the blood, absorbing nutrients through the gut and generating waste products and exchanging oxygen and carbon dioxide through the lungs,” he added. “Some of these patients also show increased blood pressure and heart rate in response to surgical incision. And, finally, more dramatic examples include sexual maturation in children and gestation of a fetus in pregnant women. ... For these reasons, many scholars, including myself, have concluded that ‘brain-dead’ patients are biologically alive.”
If this scientific criticism of brain-death diagnoses is accurate, then it follows that organ removal causes the biological death of the donor.
“In other words, we do not follow the dead-donor rule in practice now,” Nair-Collins added.
But stopping the procurement of organs from “brain-dead” donors, on the grounds that they are really still alive, would exacerbate the organ shortage for transplant, he said. So, he said, doctors alternatively could “make exceptions to the dead-donor rule ... but to explicitly acknowledge that organ donation causes the biological death of these patients.”
Defining Death Downward
The Internet survey’s findings add to a growing number of studies and commentaries advocating replacing the requirement that organ donors be “biologically dead” with the idea that organ harvesting be based on consent to death by donation of vital organs.
Chief among those advocating for reform is National Institutes of Health ethicist Franklin Miller, author of the 2011 book Death, Dying and Organ Transplantation: Reconstructing Medical Ethics at the End of Life.
Miller also published a paper in the Journal of Medical Ethics last year entitled, “What Makes Killing Wrong?” He answered that it is “not that the act causes loss of life or consciousness, but, rather, that the act causes loss of all remaining abilities.” Death is merely “irreversible, total disability,” he contended. “Death is still distinct from total disability, but it is no worse.”
Therefore, he argued, it isn’t “morally wrong to kill patients who are universally and irreversibly disabled, because they have no abilities to lose. Applied to vital-organ transplantation, this account undermines the dead-donor rule and shows how current practices are compatible with morality.”
The case of Jahi McMath, a 14-year-old California girl whose mother is fighting her diagnosis of “brain death,” illustrates that defining death is not always clear-cut. But rather than pausing organ donation in such cases of questionable death, Miller argues instead for taking organs from living patients on grounds that they are totally disabled and have nothing to lose.
‘Gray Magic’
Robert Truog, professor of ethics, anesthesiology and pediatrics at Harvard Medical School, also favors doing away with the dead-donor rule to allow procurement of vital organs from living patients. “Are we gerrymandering the lines between life and death solely to meet social goals, as important as they are?” he asked a convention of ethicists at the University of Chicago in 2012.
Truog highlighted problems of the modern definitions of brain and cardiac death, citing instances where people are pronounced dead — “dead enough for skin incision and organ procurement,” for example — and then recovered, on their own or with intervention. Such examples illustrate that the definitions of death are “convoluted” and “torture our commonsense understanding of what it means to be dead.” As well, he added, “Current practices violate the dead-donor rule — they’re perfectly ethical, but not because they’re conforming with the dead-donor rule.”
Widespread acknowledgement of these problems associated with the dead-donor rule “destroy the public’s trust in the organ-transplantation process, and this will lead to the unnecessary death of many patients. But we’ve got to come up with other ways of talking about it because we need to save the lifesaving enterprise of organ transplantation,” Truog said.
“What about procuring organs before death?” he asked. “We’ll call it DPD — donation prior to death.”
While medical ethics has traditionally drawn a firm line between physician as healer and physician as killer — a “line between white magic and black magic,” he said, “sociologically, we have been shifting away from that, more towards, you might say, gray magic.”
Opposing Perspectives
Proponents of “donation prior to death” might be encouraged by the apparent shift in public attitudes reflected by the recent survey, but Robert Veatch, professor at the Kennedy Institute of Ethics at Georgetown University, dismissed it as “meaningless,” since the “vignette” it described listed criteria that are “recognized as brain death in most countries of the world” and so does not represent an actual violation of the dead-donor rule.
And while doctors do make mistakes in defining brain death “all the time,” Veatch said, Truog and Nair-Miller belong to a minority of ethicists who say brain death is a complete fabrication. Unlike most of those who reject the validity of brain death, however, these ethicists advocate active euthanasia, albeit in a roundabout way.
“They don’t make an ethical distinction between withdrawing treatment and actively killing someone,” Veatch commented. “They see no difference between unplugging a ventilator to allow death to occur and killing a patient by surgically removing his lungs; both are perfectly acceptable.”
Many Catholic medical experts refer to a statement given by Pope St. John Paul II to an international organ-transplant society in August 2000, which recognizes “brain death” as a “sign that the individual organism has lost its integrative capacity” and therefore died, and organ donation is permissible.
But the Church has clearly distinguished between legitimately allowing a person to die by natural causes when withdrawing “extraordinary” support and the grave sin of intentionally causing death by harm — surgical or otherwise.
And regarding the notion of DPD, the Church is unequivocal: “Individual vital organs cannot be extracted except ex cadaver,” declared Pope Benedict XVI in 2007. That papal statement echoes the Compendium of the Catechism of the Catholic Church, which states, “The principal criteria for the life of the donator must always prevail so that the extraction of organs be performed on in the case of his/her true death” (47c).
Furthermore, while the Catechism of the Catholic Church states that organ donation after death “is a noble and meritorious act,” it also specifically instructs that “it is not morally admissible directly to bring about the disabling mutilation or death of a person, even to delay the death of other persons” (2296).
Belgium and the Netherlands
However, in two European countries that have legalized euthanasia, organs are already being removed in apparent contravention of the dead-donor rule.
In Belgium, organs have been harvested for several years from patients killed by lethal injections administered by doctors. And in the Netherlands, two leading medical institutions have drafted national guidelines regulating similar donations from persons euthanized there, Mercatornet reported Dec. 1.
Prominent euthanasia opponent Wesley Smith condemned the development in a Nov. 26 entry at his Human Exceptionalism blog. Such state-sanctioned actions, he contended, have the effect of persuading disabled or mentally ill persons that “their deaths have greater value than their lives.”
Commented Smith, “Belgium and Netherlands are off a vertical moral cliff. Logic dictates this is where we will go, too, if we decide to follow them into the abyss.”
Celeste McGovern writes from Scotland.
Register staff contributed to this report.
- Keywords:
- brain death
- celeste mcgovern
- euthanasia
- jahi mcmath
- martha perez
- organ donation
- wesley smith