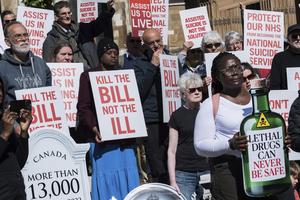Court Bars California From Forcing Conscientious Objectors to Participate in Assisted Suicide
The lawsuit, filed by ADF attorneys on behalf of Christian medical professionals in February, concerns California’s End of Life Option Act, which legalized physician-assisted suicide in that state and went into effect in 2016.

A federal district court ruled Sept. 2 that California — temporarily — cannot force medical professionals to participate in assisted suicide against their conscience.
The U.S. District Court for the Central District of California granted a preliminary injunction in Christian Medical & Dental Associations v. Bonta, prohibiting California officials from enforcing a provision “which requires a health care provider who is unable or unwilling to participate to ‘document the individual’s date of request and provider’s notice to the individual of their objection in the medical record[.]’”
Documenting a patient's request for assisted suicide would fulfill the first of two oral requests required for a patient to undergo assisted suicide in that state.
“The court also clarified that the law doesn’t require [medical professionals] to refer for assisted suicide, or to provide information about it because that would violate their medical ethics and religious convictions,” Kevin Theriot, senior counsel for the faith-based legal organization Alliance Defending Freedom (ADF), told CNA.
The lawsuit, filed by ADF attorneys on behalf of Christian medical professionals in February, concerns California’s End of Life Option Act, which legalized physician-assisted suicide in that state and went into effect in 2016. Following the act’s passage, California legislated not only to eliminate important safeguards from the act, but also to force physicians to participate.
With the preliminary injunction, the court decided that the medical professionals “are likely to succeed on the merits of their First Amendment free speech claim.”
Theriot, who argued on behalf of those challenging the California law, interpreted the court’s decision.
“Practically speaking, when a court does that, then the fact that you’re likely to succeed almost always means that you will,” he said.
“It means that we have succeeded while the case is pending,” he added of the preliminary injunction. “That’s important to know, that for physicians in California…the law is put on hold so that they’ll be able to live out their beliefs without fear of the government punishing them while this case is going on.”
He said that the case concerns both freedom of religion and freedom of speech.
“We won on our free speech claim. The court said that you can’t compel a physician to violate their convictions by speaking in a way that is contrary to their beliefs,” he said. “But we also have a free exercise claim — and the court didn’t award the injunction based upon that claim — but we’re hopeful and confident that courts will recognize that this also violates freedom of religion and free exercise rights.”
While Theriot is unsure when the case will be resolved, he anticipated a possible hearing next year on making the preliminary injunction a final one.
“Health care professionals shouldn’t have to live in fear of government punishment when they’re living according to their beliefs,” he urged.
The preliminary injunction comes after ADF attorneys representing a Christian doctor and the Christian Medical & Dental Associations asked the court to halt enforcement of California’s law, while their lawsuit proceeds, according to a press release.
Among other things, while granting the preliminary injunction, the court found that the “documentation requirement imposed by the Act ‘plainly alters the content’ of non-participating health care providers’ speech.”
“Non-participating providers, who oppose assisted suicide, are required to make a notation in an individual’s medical record ‘document[ing] the individual’s date of request and provider’s notice to the individual of their objection,’” the court order reads. “This documentation can then be used to satisfy one of the two oral requests required to obtain aid-in-dying medication.”
The court order adds: “The ultimate outcome of this requirement is that non-participating providers are compelled to participate in the Act through this documentation requirement, despite their objections to assisted suicide.”
In response to a request for comment, the office of the attorney general of California — Rob Bonta, who listed as a defendant in the lawsuit — told CNA that it is reviewing the decision.
- Keywords:
- assisted suicide