Who Guards the Gards?
COMMENTARY: Deciding what is in the best interests of infant Charlie Gard.

Sometimes the plight of one child, or of one family, captures the imagination of the world.
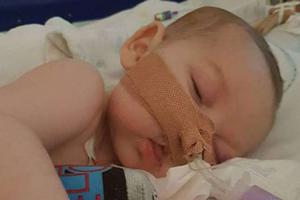
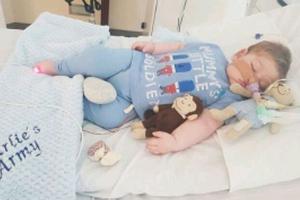
The poignant case of Charlie Gard, who suffers from a rare form of mitochondrial disease for which there is no known cure, has reminded us of the preciousness of every life, no matter how frail and brief in span.
Some comments, including some by doctors, have failed to appreciate this value. The anguish and commitment of the parents has also touched millions and elicited statements of solidarity from all over the world, not least from Pope Francis.
The suffering of the parents in this case has been compounded by a dispute over what treatment would be in Charlie’s best interest. The doctors caring for Charlie want to withdraw ventilation and provide only palliative care. The parents want to take Charlie to the United States for experimental “nucleoside” therapy and have raised more than 1 million pounds (nearly $2 million) through crowdfunding to make this possible.
The failure of the two sides to agree has led to a succession of legal judgments by different courts, each of which, thus far, has found against the parents.
The legal case was initiated by Great Ormond Street Hospital, where Charlie was being cared for. The hospital sought a declaration that it would be lawful and in Charlie’s best interest for artificial ventilation to be withdrawn; for his treating clinicians to provide him with palliative care only; and for Charlie not to undergo nucleoside therapy, provided that whatever treatments were given would be “the most compatible with maintaining Charlie’s dignity.”
Note that the issue was not about whether Charlie was a human being worthy of respect. The question was, rather, what treatments would be in Charlie’s best interest, given his present condition and the likely benefits and burdens of treatment.
The doctors caring for him thought that ventilation and suctioning were probably causing Charlie distress. Given that Charlie’s health was deteriorating with no reasonable hope for improvement, they considered that the time had come to withdraw invasive procedures and to concentrate on palliative care. The doctors also considered that nucleoside therapy had no realistic prospect of benefit for Charlie’s condition.
Note also that the case was not about the provision of food and fluids, which, in the words of Pope St. John Paul II, “always represents a natural means of preserving life” and “should be considered, in principle, ordinary and proportionate, and as such morally obligatory” (while they are still providing nourishment or alleviating suffering).
The issue of nutrition and hydration was not raised by either side at any stage in the court proceedings.
The issue was, rather, that of artificial ventilation and suctioning, forms of treatment that, according to Pope Pius XII, “go beyond the ordinary means to which one is bound,” such that “it cannot be held that there is an obligation to use them.”
Of course, in an individual case, artificial ventilation might be medically indicated and proportionate, but, in general and for the most part, such interventions do not have the same symbolic or moral significance as giving food and drink. If a patient is in terminal decline then it is prima facie reasonable to ask whether ventilation is still appropriate.
The position of the Anscombe Bioethics Centre is that to withdraw ventilation and not to seek experimental treatment “are decisions that parents in this situation could reasonably make on behalf of their child. The decisions themselves are morally defensible. The Catholic moral tradition does not oblige the use of medical procedures that are burdensome, dangerous, extraordinary or disproportionate to their expected outcome.”
There is, however, another aspect of this case that raises concerns — not that the final decisions were unreasonable, but that the courts did not show sufficient respect for the presumptive right of Charlie’s parents to decide what was in his best interests.
Arguably, the courts acted on behalf of Charlie, and thus in the place of his parents, without on each occasion having shown that the parents were being so unreasonable that the decision had to be taken out of their hands. Where the actions of a parent are likely to lead to serious harm, or where parents cannot agree between themselves, then family law has its place.
However, it is contrary to natural justice for the state to substitute for the role of the parents unless the parents are shown to be putting their child at risk of significant harm.
Regrettably, the Court of Appeal did not consider the reasonableness of the parents’ decision, but made its own independent assessment on the balance of the advantages and disadvantages of the medical steps under consideration. This approach treated Charlie as if he had no parents and Charlie’s parents as though they had no natural authority to speak for their own child.
In the view of the Appeal Court, undertaking nucleoside therapy would have subjected Charlie to the risk of significant harm because it would involve the burdens of ventilation, in addition to possible side effects of the nucleoside therapy itself. However, the only known side effect of the therapy itself is diarrhea, and this could have been controlled by reducing the dose. Furthermore, the burden of continued ventilation would be limited if the therapy were given for a trial period.
At the outset of the court case, the parents argued that they were only seeking a chance to see whether nucleoside treatment might work. The father testified that, “after three months, we would want to see improvement and, if there wasn’t, we would let go.”
It should be noted that, by taking this case to court, the doctors have had to subject Charlie to ventilation for more than three months and have subjected the parents to further distress, without any realistic chance of long-term benefit for Charlie. Had the doctors allowed Charlie to be transferred to another medical team who were prepared to provide nucleoside treatment for a trial period, and had Charlie’s condition failed to improve, then by this point the parents might have been reconciled to the transition to palliative care. Transferring his care would not necessarily have exposed Charlie to a greater risk of harm than the risks involved in taking the case to court.
There is another irony here in that, whereas the U.K. courts showed little if any latitude in relation to parental authority, the final decision the European Court of Human Rights was based on just such latitude in relation to the authority of the U.K. courts.
“The [European] Court bore in mind the considerable room for maneuver (‘wide margin of appreciation’) left to the authorities in the sphere concerning access to experimental medication for the terminally ill and in cases raising sensitive moral and ethical issues, reiterating that it was not for the court to substitute itself for the competent domestic authorities.”
The European Court was right to recognize that it is not for a higher court to substitute for a competent domestic authority. However, by the same logic, it was not for the U.K. courts to substitute for the competent natural authority of the parents. Their judgment may sometimes need to be corrected, but they should always be the first judges of what is in their child’s best interests.
David A. Jones is the director of the Anscombe Bioethics Centre,
a Catholic think tank in Oxford, England.
- Keywords:
- charlie gard
- dignity of human life