Jahi McMath Dies Four Years After Being Declared Brain-Dead
The teen defied the medical definition of brain death, and her family’s fight to spare her life has fueled other challenges to this complicated medical diagnosis.

Nailah Wakefield spoke to her daughter for the last time June 22 — four and a half years after five doctors had declared Jahi McMath brain-dead.
I said, ‘Jahi, if you’re tired, you don’t have to do this for me. … You have my permission; you can go.’”
Jahi, 17, who ignited a firestorm of mistrust about what doctors have called “brain death,” died a few hours later. She had undergone surgery that day, but she was still on the respirator that had become the center point for the debate between ethicists, doctors and a wide following of observers over whether or not she should be considered alive.
“You can still die on a ventilator,” Wakefield, the teenager’s grieving mother, who fought for years for her daughter to remain on the machine, told a news conference after her daughter died. “There’s not a machine in the world that will keep you alive if God wants you. He is going to come get you. I’ve been saying that since Day One.”
Day One was Dec. 9, 2013, when McMath entered Oakland’s Children’s Hospital for a routine tonsillectomy but began bleeding profusely from complications that her family says were ignored for hours. Then 13, the Oakland girl suffered a heart attack.
Two days later, the doctors declared her brain-dead. Hospital staff approached the family to ask for her organs. Wakefield and her family refused and called personal injury lawyer Christopher Dolan.
Through the legal battle that ensued, five doctors in the state of California confirmed the first diagnosis — which signifies “irreversible cessation of all functions of the entire brain, including the brain stem,” according to the Uniform Declaration of Death Act.
However, Dolan won the family the right to take McMath to the state of New Jersey, the only state which recognizes “religious” objections to the brain-death label, where she was cared for at St. Peter’s University Hospital in New Brunswick, which is run by the Diocese of Metuchen, and subsequently transferred to a private home to be cared for by her family.
Though they had plastered Jahi’s walls there with cards from well-wishers, Wakefield said she was lonely while taking care of her daughter and had received death threats and seen insults to her daughter online while the controversy played out in the news. Leading ethicist Arthur Caplan, for example, had called the young teenager a “corpse” and said that she was “going to start to decompose” and that “keeping her on a ventilator amounts to desecration of a body.”
‘She Was Always Alive’
“There’s no way in the world that I would be holding onto a corpse,” Wakefield said at her news conference. “When I got to New Jersey, she was only 13, and I watched her become 17 and a half. She grew taller, and her features started to change — and she went into puberty and everything — and I know for sure dead people don’t do that.”
Added Wakefield, “She was always alive.”
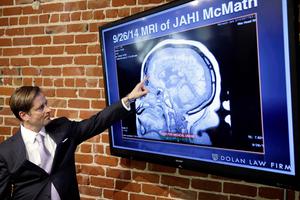
Wakefield said she was able to communicate with her daughter with subtle finger and other movements on command. Videos of this were released, and in 2015, neurologists said that while doctors had correctly diagnosed Jahi as brain-dead, she had improved and was no longer dead — a first in the legal history of brain death.
After her death last month, the state of New Jersey issued a second death certificate June 22 for the teen whom the state of California issued a death certificate for in December 2013.
Wakefield said she was sorry that her daughter had to die so far from home, where she should have been surrounded by more family and friends.
At the news conference, she called on others to “stop letting the doctors tell you to prematurely disconnect your family members. … Do not let the hospital bully you.”
“I hope the fight that I put up opened a door to help other people,” she said. “I know that they [in California] didn’t want her to live; they didn’t want her to beat the odds. But that little black girl from Oakland made history, and I’m so proud of her. She’s beautiful. Even when she wasn’t saying a word, Jahi really had the whole world stirred up. … She lay in a bed with her eyes closed in silence and had everybody talking about her in different parts of the country. That’s powerful.”
Canadian Cases
Others have been inspired by the McMath family’s battle. The family of Taquisha McKitty, a 27-year-old Ontario woman declared brain-dead by Canadian doctors in September following a heart attack that resulted from a drug overdose, challenged her diagnosis in court after hearing of McMath’s case.
Like McMath, McKitty menstruated and continued to show other signs of life, including crying and healing from injuries. “They said her brain would liquefy; it hasn’t happened,” her uncle told reporters.
Four days after McMath’s death, however, an Ontario Superior Court of Justice ruled that McKitty should be considered dead and can be removed from life support.
“There is no legislation that requires physicians to consider an individual’s views, wishes or religious beliefs as factors to be considered in the determination of death,” Justice Lucille Shaw wrote in her 111-page judgment. The family was given 30 days to appeal the decision, which may be precedent-setting on the Canadian common-law definition of death, religious beliefs and the Canadian Charter of Rights and Freedoms.
Stanley Stewart, McKitty’s father, said the decision is “basically giving doctors the power to play God” and that the family may appeal within the allotted 30-day window.
“It leaves the determination of death exclusively to doctors, without any means of oversight or consideration of the protections or values of the Canadian Charter,” Hugh Scher, the lawyer representing McKitty, said to reporters after the decision was handed down.
Scher is also representing a family in the similar case of Shalom Ouanounou, a 25-year-old Orthodox Jewish man who was declared brain-dead at Toronto’s Humber River Hospital following a severe asthma attack.
Ouanounou’s family sought an injunction at about the same time as McKitty’s family launched their fight, arguing that he should be kept on life support in recognition of their Jewish law that stipulates death is defined by absence of a heartbeat.
Ouanounou stopped breathing and was put on life support in March. The Ontario Superior Court has yet to rule on the family’s legal arguments.
Legacy
For decades, the Church has deferred to doctors to define and diagnose brain death. Catholics frequently refer to St. John Paul II’s remarks in 2000, when he commented that the definition of brain death, “if rigorously applied, does not seem to conflict with the essential elements of a sound anthropology.”
At the same time, the Church has endorsed Catholics in either decision to use or not use “extraordinary means,” including ventilators, to support loved ones; they are not morally obliged to do so and are to be supported if they choose so.
Whether the life and death of Jani McMath will have a bearing on Catholic teaching remains to be seen. But it has already had an influence on how some brain-death diagnoses are received in the United States.
“I think the legacy of the McMath case, at this point, is the heightened awareness it has raised about this issue and the potential willingness of families to challenge the legal status of the diagnosis of brain death,” Robert Truog, director of the Center for Bioethics at Harvard Medical School, said in an emailed statement to the Register.
He added that there are “at least 8,000 cases annually in the U.S. — that’s the number of patients who agree to donate their organs and does not include many others in whom the diagnosis is made who either are not candidates for organ donation or who decline to donate.”
Celeste McGovern writes from Berwick, Nova Scotia.
- Keywords:
- brain death
- celeste mcgovern
- jahi mcmath